HDU
29 September 2009
Luke might be moving out of PICU into HDU (High Depependancy Unit) soon whilst he awaits his next operation. It is a step forward to go to HDU but Luke is a bit worried about leaving all the super professional nurses and doctors that he*s made friends with.
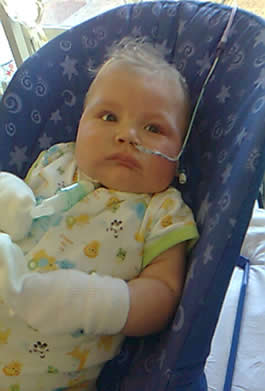
daddy gets cuddle!
28 September 2009
Daddy managed to get his first cuddle for a long while yesterday of which he hopes will be the first of many!
Luke seems to be doing better recently, coping more with being a baby but he is still very agitated from the Morphine and Clonodine withdrawal.
He still needs to have an operation to have his bowel resected sometime soon.

bath time!
25 September 2009
Lukes not been able to have a proper wash for weeks but yesterday he had a nice bath he wasn*t sure what to make of it all at first and had a little grump, but he soon remembered he likes bath time and was all sparkling clean again.
.jpg)
sleepy dust
23 September 2009
Enjoying a mid morning snooze in my chair after a good night.
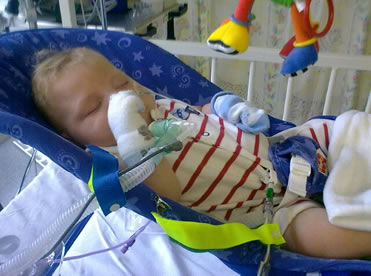
Later on we had some smiles!
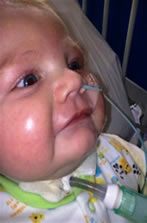
Chair
22 September 2009
Today Luke had a relax in his chair, he likes the chair (even though he looks a bit grumpy here) because it means he can look around and keep an eye on whats going on...
Meanwhile life back home is a bit quiet and PlopZilla has resorted to eating pot-noodles and reading FHM!


Nippy
21 September 2009
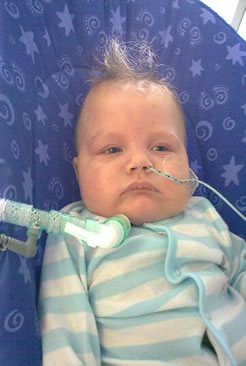
Luke seems to be making progress at last. For the last few days he has been on a NIPPY which is a small portable ventilator which is a big step forward long term.
Luke had cuddles today, the first time for over a month for which most hes spent drugged out of his brains on morphine, completely asleep. For a tiny baby not to be able to near its mother for such a long time is truly sad - but today we had some smiles!
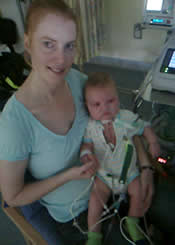 (the NIPPY is the white box on shelf in background)
(the NIPPY is the white box on shelf in background)
FUNDRAISING FOR PICU
21 September 2009
Daniel Broom (Lukes Uncle) will be running the Great South Run in Portsmouth on 25th October hoping to raise money for the Paediatric Intensive Care Unit (PICU) at Southampton General Hospital. The Charity is special to him as it saved the life of his nephew, Luke, who was admitted to the unit in June with a congenital diaphragmatic hernia. The condition, which can be fatal, affects 1 in 5,000 babies and is normally diagnosed at or before birth. Luke was only 6 weeks old when he became critically ill and it took all the expertise of the staff on PICU to save his life during emergency surgery. Since then, Luke has had 8 operations, including having his right lung removed, and although his condition has started to improve, he still remains critical, on a ventilator on the PICU ward. With at least one other operation still to come, Daniel and his family remain extremely grateful to the commitment of the PICU staff who are continuing to work hard to support Luke and aid his recovery.
PICU is the regional centre for the South of England, and one of only 9 tertiary care centres in the UK. This means that any child needing intensive care in the South of England would be likely to receive treatment there. As there are only 11 purpose built bed spaces, the unit can become full quite quickly. More than 700 children are admitted each year, many from A and E departments across the region or following major surgery. Children from newborn to 17 years are cared for in the specialist unit. This may be due to massive trauma following a road traffic accident, or other serious illnesses, or as a result of serious heart disease in tiny babies. The unit encourages family centred care by incorporating the family in the care of their child, and providing family accommodation to help the families cope with the trauma of their child being admitted to the unit.
Running such a service requires high standards of care, and this requires frequent investment. The charity, Friends of PICU, aims to support this work by helping to purchase new life saving equipment, as well as toys, baby equipment and in the near future a new ambulance. The average cost of a night on the ward before any medical intervention is £1500, whilst the incubator that Luke first stayed in cost £75 000 so costs are very high! If you would like to support this Charity then please log onto Daniel’s web page: http://www.justgiving.com/Daniel-Broom/
aorta pexi
16 September 2009
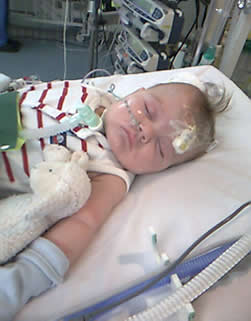
 Luke had his 8th major operation yesterday an Aorta Pexi in which they had to crack open his sternum and suture (stich) his aorta to his sternum to relieve the pressure of it on his airways.
Luke had his 8th major operation yesterday an Aorta Pexi in which they had to crack open his sternum and suture (stich) his aorta to his sternum to relieve the pressure of it on his airways.
The op seemed to go well, the general feeling was that it needed to be done and should achieve some greater good both long and short term.
Unfortunately in the operation Luke dumped out quite alot of blood and fluids so when he arrived back in PICU he had to be given a top up of blood and Gello (plasma type of thing) Later on that evening he continued to look very pale, his lips losing all redness and his blood pressure seemed to be dropping quite rapidly even though they were keeping him topped up with fluids. After an X-ray one of the consultants noticed some fluid build up around his lung and decided to put another chest drain in to remove it. This did not seem to work as the blood had coagulated and would not drain out, so this moring he went in for a mini op to remove and this seems to have gone ok and Luke is now back on PICU after operation number 9!
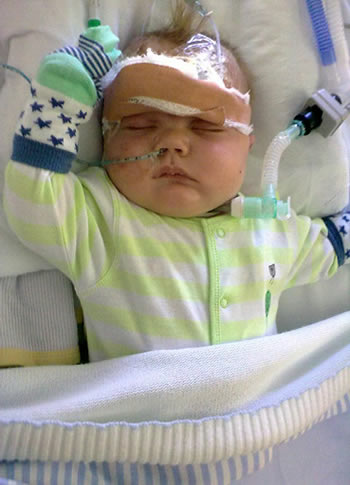
Ram-baby
14 September 2009
Luke has had quite a settled weekend all but for knocking the cannula out of his head causing a loss of blood so he had to be bandaged up like Rambo which I think he will proud of when hes older!
His pressures have been good over the last few days, down to 13 at some points and being under 20 most of the time.
We are hoping he will be ok for his Pexi op tomorrow morning.
line infection
11 September 2009
Whilst going through the consent form and checklist for his op they realised Luke had a line infection so now looks like no op for today (friday) :( . Better to be safe than sorry and we understand the concerns of PICU - its just a bit gutting to have more set backs and more bad luck for Luke...
His op will now be on either monday but probably tues so hoping he will get through weekend ok.
Yesterday was an ok day, his peak pressures came down a bit to mid/late twenties. They shaved his head and put line in and I got told off from mum for letting them throw a bit of his hair away... :/
ok ish night
9 September 2009
Luke seemed to have had an ok night with no major death episodes.
The new plan is for a mediastino pexi on Friday. This operation basically involves moving and stiching the heart ot the inside of the chest cavity and some general rummaging around to see if they can make his airways less distorted.
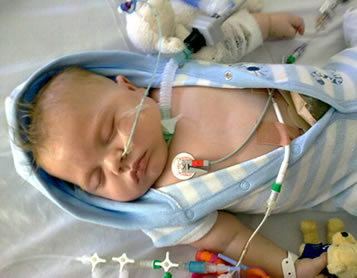
up and down
8 September 2009
After seeming to make some progress yesterday with his pressures being in the high teens and Co2 levels coming down, and him even being out of cot for a cudddle, in usual style Luke has decided that after a good day a bad night must follow.
During yesterday he was vomiting and did not seem himself in the afternoon.
In the night he had to be bagged (mainly thought due to a secretion plug in airway) and his pressures are back up around 30 when we would like them to be low twenties.
At the moment hes on Midazolam rather than being veced out and about to have some physio on his chest.
Co2 Improve?
6 September 2009
Luke had an ok ish night with only one minor episode at about 4am. For most of today he has been allowed to be awake and sems to be quite happy. In fact I have noticed have noticed his Co2 levels have dropped a little over the last few days and today he did not need to be veced out while he was awake and his PEEK pressure dropped to 18 at one point and hovered around 20/23 which is the best its been for weeks. I am wondering if this is anything to with him turning his head more to the center when I was playing with him making the airway clearer - and of course hopefully getting a bit better too!
Blood Transfusion & PEEK
5 September 2009
A relatively ok day for Luke until about 5:50pm when he woke up coughing, had a minor death episode and had to be bagged and Veced out (put out of it).
Nanny & Nanny NuNu both came to visit in afternoon.
During the last few days Lukes blood hemoglobin content has become a bit low due to all the samples taken for test to make sure everythings ok. This means the blood is not carrying oxygen as effeciently as one would like. It sould be at 11 and never really go below 7.2 his has been at 7.2/7.3 for the last few days as his body can not regenerate it quck enough as hes so small - thus a blood transfusion was given today at about 6pm and it seems to have gon ok with no reactions etc.
PEEK
Peek is the amount of air pressure being put in by the ventilator and it ideally needs to stay below 35 ideally around 23/25 - best would be low teens. When Luke wakes up it can become 35/36 which is worry as the extra pressure can damage his lung.
CT Scan Day
4 September 2009
Luke had his CT scan today. Before he was due to go in the scanner he had a minor death episode and had to have some atropine just to keep his heart rate up. This was probably caused by secretions being dislodged caused by all the moving in and out of his bed space.
We already know he has bronchial malacia in both the upper bronchus and a further narrowing far down in the lower lobe. One problem this causes is him being able to get enough oxygen to this lower lobe to help prevent infections.
The CT Scan results did not really reveal anything exciting. One hypothesis for his death episodes is that the left lower lobe of his lung is aggravating one his major arteries. Another thought is that these same arteries become enlarged because of the amount blood going through them due to the extra work he has to do only having one lung.
The doctors and consultants will meet on Monday to see if there is a way forward.
CT Scan?
3 September 2009
Luke is still in picu. Is very veced out at the moment due to the number of secretions he is producing. He has to have lots of suction to remove because he cant cough.
He is due to have a CT Scan tomorrow which we hope will show the state.
his morphne is still 1.4 - cholonodice 0.6
Tracheomalacia
1 September 2009
Any problem with the cartilage framework which normally supports the trachea will mean that the wall making up the airway is softer than it should be. If there is a long section without cartilage, this can cause a ‘floppiness’ of the trachea, and this is called tracheomalacia.
Mucus is a sticky fluid which is found on the surfaces of the normal airway. Its main function is to trap dust particles in the air, before they travel deep into the lungs. The specialised lining cells of the airway have mechanisms both to produce this mucus, and then to transport it - together with the trapped dust particles - up the airway to the throat, where it is either coughed out or swallowed.
The mechanism is normally so efficient that most people hardly notice that they have mucus to clear and just automatically clear their throat from time to time.
Severe tracheomalacia
In extreme cases, the infant may experience acute life-threatening episodes often called ‘near death episodes,’ when the baby seems to be choking and unable to breathe. The trachea actually collapses, so that no air can pass through it.
Because these extreme situations are so rare, many doctors have never witnessed one of these episodes; the child is in any case often perfectly well by the time they get to hospital or are seen by a doctor.
The story of a baby going blue with hard crying may suggest ‘breath holding attacks’ - which are relatively common. However, these tend to occur in older toddlers who are either angry or very upset, and happen at the end of a big breath in or out. The ‘near death episodes’ usually happen in the midst of a normal crying spell, and happen near the start of either breathing in or out (depending on where the tracheomalacia is). Observers who can describe these kinds of detail about episodes can help greatly in making a correct diagnosis.
The attacks can be very distressing. Nonetheless, when the child passes out, their relaxed state helps to open up the airway, bringing recovery; gently pulling the tongue forward may help as a first aid measure. If the baby is unconscious and not breathing, blowing gently into the airway by mouth to nose-and-mouth respiration is the correct course of action.
Drugs used on Luke
5 September 2009
MORPHINE - Sedative
CLONIDINE - Helps with the withdrawal of long term Morphine use and high blood pressure.
VECURONIUM - A muscle relaxant in the category of non-depolarizing blocking agents.
MIDAZOLAM - fast acting short term pain killer
CHLORAL HYDRATE - A sedative and hypnotic drug as well as a chemical reagent and precursor.
SUXAMETHONIUM - A medication used to induce muscle relaxation
PIRITON - stops itching caused by morphine
PARACETAMOL - General pain killer
PETHADINE -
SODIUM HYDRATE -
VAMIN -
LIPID -
Lukes Operations
23 September 2009
Luke has had to have many different operations, scans and checks.
- aorta pexi - involves cracking open stenum for some general rumaging about with heart and airways
- laparotomy - involves an incision through the abdominal wall to gain access into the abdominal cavity
- CT Scan - a special kind of X-ray machine. Instead of sending out a single X-ray through the body
- bronchoscopy - a procedure which can help to diagnose some conditions of the airways (bronchi)
- thoracostomy - involves making an incision between the ribs (under the armpit)
- pneumonectomy - the surgical removal of a lung
- tracheostomy - a surgical procedures on the neck to open a direct airway via an incision in the trachea